Many Americans feel very stressed, and a lot of people worry about burnout at their jobs. While I sympathize with those schedules and stressors, there are a few jobs that are in a different class all together. I have counseled thousands of people from all types of vocations, but over the last decade, I have done a lot of work with law enforcement officers, correction officers, current service members and veterans, and social workers. These are high stress jobs that affect both the workers and their families. I have a very strict definition of a high-stress job (full disclosure: none of my work meets my criteria for high stress). It means:
A) one’s physical safety is under regular or constant threat
and/or
B) one sees/deals with horrible things happening to people under 18 years old
To be clear, horrible things can mean malnutrition, verbal abuse, physical abuse, sexual abuse, burning, mutilation, and/or death.
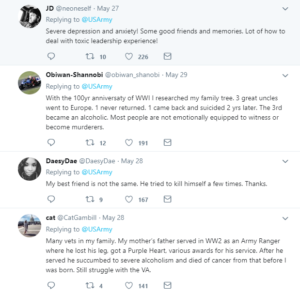
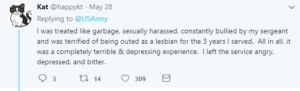
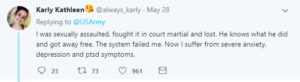
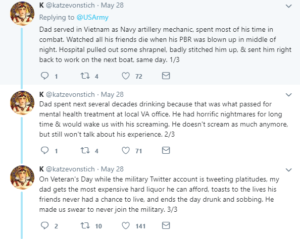
Most correction officers meet the criteria for A. Many law enforcement officers do as well. Some service members do. Social workers who are working in prisons or child protective service agencies certainly do. PTSD or complex PTSD (C-PTSD, which the public and even most professionals don’t know about) are more common than not in people with those jobs who meet criteria A.
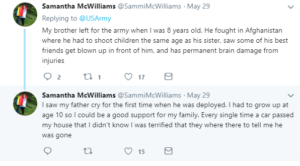
Unless the correction officers work in a juvenile detention facility, they won’t bump into criteria B. Law enforcement does, particularly those who deal with domestic violence calls, car crashes, and most horrifically, child sex crimes. Almost all child protection service workers come across neglect and physical abuse, and many have to deal with the fall out from sexual abuse. Those who are in the military and come upon dead children in war zones are usually haunted by those images (I’m not even going to write about those who had to take the life of a child soldier or child suicide bomber, as I doubt I have the power to explain that situation to civilians). In the summer of 2017, I spent some time talking to an Army sniper who worked as a fire fighter when he wasn’t on active duty. He told me about how difficult it was to come across the bodies of burnt up children. I asked him how common it was. He said it didn’t happen much, but that most firefighters he knew that spent 20+ years on the job had seen that. Of course, I asked him if he or other firefighters had a chance to process it with a therapist who understood trauma. He laughed and said, “Of course not.” To be clear, anyone who meets criteria B over a sustained period of time is very likely to have symptoms of PTSD or C-PTSD.
I have grave concerns for these professionals and public servants, because their work is vital to our society. They are the ones with their hands in the muck. And the work does a number on them and their families. And their families. The jobs can be overwhelming, and there usually isn’t mental health and community support to deal with the side effects of the work.
In the aforementioned professions that meet one or both of the criteria, the following conditions are more common than in the general population:
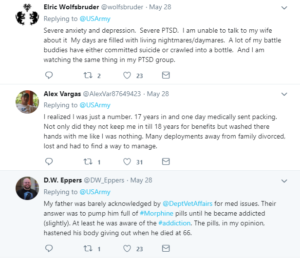
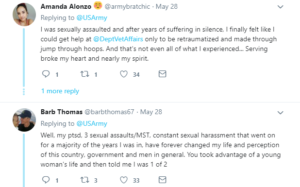
substance misuse, anxiety, depression, PTSD, C-PTSD, disorganized gambling disorder, suicidal ideation
Those public servants are also more likely to have poor spending habits (using money to feel better), act out sexually, put themselves in dangerous situations (driving a motorcycle with a helmet, engaging in extreme sports, going into buildings without backup), isolate at the end of the day, and have marriages that end in divorce.
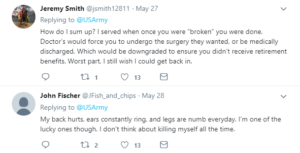
Because most are in jobs where being tough is a value, therapy is usually not offered and often looked down upon. “People who go there are weak” I often hear or “Other people have it worse.” I tell them if they meet the criteria for A or B, that very few people actually have it worse. They usually don’t tell their spouses about their work. They might utter “rough day” or “the usual” or “you don’t wanna know” or just sigh and go silent. Some variation.
The job changes them (how can it not?). They become quicker to anger and quicker to isolate. Spouses may resent how their partner has changed. And their partner doesn’t know how to explain it. And there is a strong chance that they aren’t any good at listening to their spouse talk about their less stressful job.
To be clear, I’m not asking spouses and family members and friends to excuse bad behavior that these professionals use as coping skills. I don’t want you to be their therapist. I just want you to understand that the work is horrifying. Here is what you can do:
1) Encourage the professional to go to therapy. Continually. They need at least one person in their life that they can process these terribly experiences with continually.
2) Monitor their sleeping and eating.
3) Encourage them to exercise regularly.
4) Monitor their substance intake.
5) Come up with a way for them to signal to you that they had a particularly rough day on the job.
6) Try to understand that they will probably be poor at listening to you talk about the stressors of your job and day. This is often a common complaint from couples where one person is in a high stress job.
7) For those of you that are spouses, it is imperative that you spend time together outside of the house, at least two days or nights a month. This is important for both their stress level and your relationship (all too often, a decade into a romantic relationship, it seems like you are running a daycare/housing/taxi service with no downtime for yourselves or each other…this leads to stress, resentments and potential awful fights).
I’ll get back to this before the end of the summer. For those of you that are friends of someone in those jobs, you can play a significant part in their well being. Please do so.