by Anthony Gallo
Forward
The following article is based upon an interview conducted by the writer with an individual who served a brief sentence in federal prison. It describes the feelings of disenfranchised grief experienced by this individual after his release. All names have been changed to protect the individual’s identities. Due to a dearth of scientific research on disenfranchised grief in this context, many of the opinions expressed are based upon anecdotal evidence and extensions of related theory developed in other contexts. The article serves as an introduction to this form of disenfranchised grief for both the counselor and the ex-offender, as well as a call to action in expanding research on this topic.
Coming Home: Disenfranchised Grief
Unable to sleep, John stared up at the ceiling feeling the strangely soft sheets against his skin. The room was quiet, and the night was uncomfortably still. John thought of the men he considered brothers, sleeping far away in less luxurious accommodations. The brothers he had left behind, who had grown to know him better than anyone had before. Though he had to go, John still felt pangs of guilt for leaving. Everyone told him how lucky he was to be out, but he wanted to go back. A tear trickled down his cheek. “What is wrong with me?” he thought as his mind raced back to the night before, when his brothers and he celebrated his last night being “down.”
Suddenly the bed rustled, and John glanced over at Jenna, the woman that he loved, sleeping peacefully at his side. She had stayed with him through thick and thin, to the envy of his friends, and faithfully visited every two weeks. Now they were finally reunited, in a luxurious resort no less, yet John only felt sad and alone that night. He thought of waking her and sharing how he felt, but she was happy to have him back and he didn’t want to risk hurting or worrying her. John also knew that he could never fully convey what it was like in there, or who he had to become to survive. There were so many things John couldn’t, or wouldn’t, tell her out of fear that she wouldn’t understand.
After a sleepless night John woke Jenna and they walked together to the resort’s fitness center for his daily lifting routine. Working out was familiar, and John wanted to feel a little bit of normalcy again. He picked dumbbells off the rack, finished a set of curls, and placed them down to use the restroom. John returned to find that a man in his late sixties, with thinning white hair and a frail frame, had commandeered his weights to do lunges in the corner. Taking another man’s weight was a major disrespect and John quickly began formulating a plan to save face.
John clenched his fists as anger boiled inside of him, threatening to spill out of his mind and into action. Sensing John’s tension, Jenna tugged his arm and asked, “Is everything okay?” With Jenna’s touch the spell was suddenly broken, and John’s rage melted into shame and embarrassment at what might have just happened. John dismissed Jenna’s inquiry, afraid of what she would think if she knew that John had planned to confront this man. How could John expect her to understand his thoughts to assail someone older than their fathers over such a minor slight? John was caught between two worlds. His reaction would have made sense to his brothers but would have been deemed highly inappropriate by Jenna. John didn’t know where he fit in anymore.
Released the day before from Federal Correctional Institute Ft. Dix, John’s time being “down,” a slang term for incarcerated, was now over. John had dreamed of this day and coming home was supposed to be glorious. Yet he felt alone, depressed, and overwhelmed readjusting to society. Unknowingly, John was grieving over the loss of some elements of his time incarcerated. John kept most of this grief inside, feeling as if others wouldn’t understand or care. He was experiencing a type of grief called disenfranchised grief.
Introduced by Dr. Kenneth Doka in 1989, the term disenfranchised grief refers to any grief that falls outside the norms and rules that society sets for which losses are appropriate to mourn, who can mourn them, and for how long the losses can be mourned. For example, society would allow someone to mourn the loss of a spouse but generally would not accommodate someone’s grief over the death of a mistress or lover. While the relationship with a spouse is accepted to be legitimate and significant, a person’s relationship with a lover or mistress is taboo and therefore unacceptable to grieve over. Grieving over the return from incarceration generally falls outside the norms of acceptable grief in our society as well.
Despite having goals of reforming the inmates they house, prisons are generally regarded as horrible places that subject inmates to purely punitive and negative experiences. Few people choose to go to prison and many spend significant resources in the fight against being incarcerated. Incarceration physically restricts an individual’s freedom, puts employment on hold, removes them from their family and friends, and subjects them to elevated risks of bodily harm. Being incarcerated also often strips them of their personal identity, rights, and life purpose while drastically lowering their standard of living.
With incarceration being perceived so negatively, being released from prison is often visualized to be a wholly positive experience for the ex-offender. They have theoretically paid their debt to society and now get to return to their family and friends, re-assume their identities, regain their personal autonomy, and resume their lives and careers. They can more freely navigate the world and make their own decisions and also regain most of the rights they had prior to their time incarcerated. How then, do some inmates grieve over what should be a wonderful moment in their lives?
To answer this, we must begin by acknowledging that not all aspects of prison are bad, and not everyone has the type of traumatic experience that society expects to befall them while incarcerated. This is not intended to minimize the negative impacts incarceration has on many inmates’ lives or to justify the major issues caused by the US prison industrial complex, it simply recognizes that some inmates may find parts of their experience to be positive and fulfilling. Ignoring this fact leaves little room for understanding or empathizing with the disenfranchised grief experienced by some inmates returning to society.
In 1943, an American psychologist name Abraham Maslow developed an overarching theory of human motivation titled the Hierarchy of Needs. Adapted to the context of incarceration, his theory helps shed light on why some inmates might miss prison. Maslow theorized that humans have different needs that must be met in a sequence he ordered by physiological needs, safety needs, love and belongingness needs, esteem needs, and self-actualization needs. Physiological needs are the biological requirements for the body to function and were viewed as essential to have met before satisfying higher needs. Safety needs refer to the protection of the human from the elements and from physical harm, while love and belongingness needs include developing friendships, intimacy, trust, and acceptance. Esteem needs include aspects such as personal dignity, feelings of competence, and status or prestige. According to Maslow, the ultimate goal of meeting a human’s self-actualization needs include achieving fulfillment “to become everything one is capable of becoming.”
John’s experience shows that prison may be capable of satisfying most, if not all, of these human needs. Physiological needs are always met, even if the food and drink are sub-standard, and safety needs are generally met via consistent housing, rules, and structure in the inmates’ lives. Many love and belongingness needs can also be met inside the prison walls, either through gang involvement or close friendships. Esteem needs are sometimes met when inmates develop valuable roles in the inmate community, either informally or via their work assignments. Lastly, self-actualization needs could possibly be met through finding one’s calling within the walls of the prison, such as the jailhouse lawyer that helps overturn his fellows’ cases.
While interviewing John for this article, he shared that he had indeed felt like all his needs, other than self-actualization, had been met while incarcerated. He never had to worry about food or shelter while incarcerated. John also shared that his love and belongingness needs had been met by the close relationships he formed with a select few of his fellow inmates; men he came to regard as brothers more than friends. John also felt that his esteem needs were met through the value he brought to the community by cooking, working in the gym, and serving as a confidant for many inmates who felt comfortable speaking with him about sensitive matters.
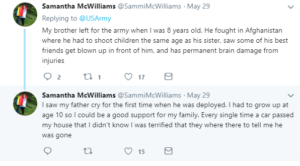
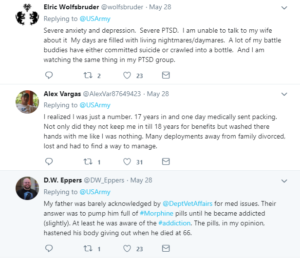
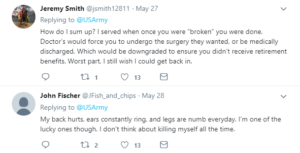
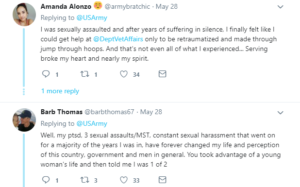
John’s physiological needs remained satisfied upon release. However, despite having a close-knit family and the presence of Jenna in his life, John consistently expressed that his love and belongingness needs went largely unmet upon his return home. To illuminate his point John made comparisons to the experiences shared by Sebastien Junger, a journalist who spent his career covering military conflict, during a TED talk on why military veterans miss war.
In the talk, Junger describes an interaction with a traumatized soldier named Brendan who had experienced death and vicious fighting on the battlefield. When asked if there was anything he missed about the war, the soldier responded, “I miss almost all of it.” Junger theorized that it was not the violence, death, or the trauma that this soldier missed, but the feeling of brotherhood he had left behind on the battlefield. Brendan missed the human connection he experienced by enduring intense hardships with his fellow soldiers, who he also came to consider as brothers. Junger went on to explain that brotherhood is a mutual agreement in a group that an individual will put the welfare of the group over the welfare of the individual. Humans are intensely social creatures and we tend to immensely enjoy such interpersonal connections. Unfortunately, civilian society’s luxuries of independence rarely afford such opportunities for true brotherhood.
John shared that he felt this sense of brotherhood amongst his closest friends in prison and he was unable to replicate it in life on the outside. John had grown to rely upon those men for his safety and emotional well-being. He trusted them to share their limited resources when in need and to expose themselves to physical danger to protect him, and they knew he would do the same in return. Spending so much time together, with nothing to do but talk, he had formed incredibly close bonds with these men and felt that they knew him better than anyone had before. When he returned home, he questioned what his friends at home would really do for him when the chips were down. How could he ever hope to feel as intense of a connection with friends who wouldn’t be willing to give their life to protect his? He wondered whether they could ever understand him and worse, whether they would judge him for the humor and customs he had developed while incarcerated.
It is not known how common John’s experience is amongst inmates returning from the criminal justice system. In researching John’s experience this writer was unable to locate any scholarly research on disenfranchised grief relating to release from incarceration. There is significant work showing the impacts of maladapted traumatic grief on incarceration and recidivism but seemingly none on the grief experienced after release. There is also much study of the similar concept of “institutionalization” but the articles reviewed largely focused on recidivism rates due to mental health, substance use, traumatic grief, and unemployment. However, this writer did find ample anecdotal evidence that John’s experience was shared by other ex-offenders by reviewing posts in online forums. The following excerpt is from one of those forum threads:
“I just think sometimes how dam stupid it all sounds…. I mean being down for 5 years in a basically max security prison and getting out and missing it. I think to myself what the hell is wrong with me? I do love my freedom I don’t want you to misunderstand me. And when I was locked up I wanted to get out so badly. And I do love life and freedom…..it’s just….I am so changed in every way and feel so alone sometimes. What’s weird though is being surrounded by people bothers me and all I can think about is leaving where I am.” – Skitten1208
John’s and Skitten1208’s experience of wondering “what is wrong with me?” struck the writer as extremely poignant examples of the difficulties posed by disenfranchised grief. When individuals experience an acceptable loss, society has already set an expectation of grief and they understand that it is okay to feel and express sadness. Additionally, they enjoy the healing benefits of empathy and understanding from friends and family, as well as an ability to engage in social mourning rituals. With disenfranchised grief there are no such expectations or emotional support for the grieving individual. These grievers therefore may not understand their grief or that their emotions are in fact natural and healthy. They may also feel intense alienation and shame for missing something that society deems that they shouldn’t.
With no research available on this specific form of disenfranchised grief, work with ex-offenders should focus on the general therapeutic concepts of treating disenfranchised grief. The counselor should stress that the grief is indeed valid, despite falling outside of societal norms, and that there is nothing wrong with the individual for grieving. Furthermore, the counselor should take time to listen to the individual and allow them to express their feeling of loss. The time in session may very well be the individual’s first opportunity to do so. It is also important that the counselor expresses an understanding of the loss through techniques such as reflecting, paraphrasing, and summarizing. The longer an individual’s grief goes without acknowledgement or legitimacy the longer it may take to resolve.
In addition to working with the affected individuals, this writer believes it is vitally important to begin conducting research on disenfranchised grief in this context. If this experience is not recognized or studied by the very professionals who make a living examining such concepts, then how can we expect impacted individuals and mental health professionals to recognize or understand it themselves? In fact, the lack of research seems to prove exactly how disenfranchised this type of grief truly is. We need to understand how common this type of grief is, how it impacts the individuals affected by it, how to treat it, and how it may play into the larger examination of recidivism in the criminal justice system.
It is this writer’s hope that this article can spur conversation and research around the topic. At the very least, the writer hopes to have shown individuals like John and Skitten1208 that there is, in fact, nothing wrong with them at all. Though society might not yet accept it, this article can play a small part in validating their experience and right to grieve.
__________________________________
Anthony Gallo is a Licensed Social Worker and Licensed Clinical Alcohol and Drug Counselor Intern with a Master’s Degree in Social Work from Rutgers University. Anthony’s experience with direct patient care complements his passion for macro social work, enabling him to promote practical legislation and outcomes focused business practices. In his personal life, Anthony is an avid auto enthusiast and enjoys theater, photography, and polishing opals.